Revision Shoulder Replacement
Revision shoulder replacement is a specialized surgical procedure performed to correct or replace a previous shoulder replacement that has failed or is no longer functioning properly. While most shoulder replacements provide long-lasting pain relief and improved mobility, certain complications or implant wear over time may require additional surgery. Revision procedures are typically more complex and require advanced surgical planning and expertise.
What Is Revision Shoulder Replacement?
Revision shoulder replacement involves removing some or all components of a prior shoulder implant and replacing them with new prosthetic parts. The goal is to address pain, instability, infection, implant loosening or mechanical failure while restoring joint stability and function. Depending on the underlying issue, the surgeon may revise a single component or perform a complete reconstruction, sometimes converting an anatomic replacement to a reverse design. This may require creating a patient specific implant or more than one surgery.
Anatomy after replacement
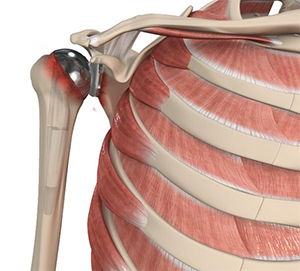
The shoulder/ball-and-socket joint has an implant in place
- The humeral head (ball) may have an implant in place
- The glenoid (socket) may have an implant in place
Over time, these implants may loosen, wear down or affect surrounding bone and soft tissue.
Pathology
Revision surgery is typically required due to complications affecting the original implant. Common problems include implant loosening, polyethylene wear, instability, infection, rotator cuff failure or periprosthetic fracture. Bone loss around the implant can also occur, making reconstruction more technically demanding. Identifying the specific cause of failure is essential for selecting the appropriate revision strategy and potential having a patient specific implant available and this may require multiple surgeries.
When Is Revision Shoulder Replacement Recommended?
Revision surgery may be recommended when a patient experiences persistent or worsening symptoms after a prior replacement, including:
- Implant loosening or mechanical failure
- Chronic pain unresponsive to conservative treatment
- Shoulder instability or dislocation
- Infection around the prosthesis
- Significant implant wear or bone loss
- Fracture around the implant
A detailed evaluation, including imaging and laboratory testing, helps determine the need for revision.
What Does Preparation for Revision Shoulder Replacement Involve?
Preparation includes a thorough orthopaedic assessment, advanced imaging such as CT scans, pulling fluid from the joint and blood tests to rule out infection. Medical risk stratification is required, and medications may need adjustment. Because revision procedures can be more complex, preoperative planning is critical. Patients should arrange postoperative support and understand that recovery may take longer than with primary replacement.
How Is Revision Shoulder Replacement Performed?
The procedure is performed under anesthesia through an incision that may follow the previous surgical scar. The surgeon carefully removes the existing implants, addresses bone loss or infection if present, and reconstructs the joint with new components. Bone grafting or specialized implants may be used to restore stability and alignment before closing the incision.
What to Expect During Recovery After Revision Shoulder Replacement?
Recovery varies depending on the complexity of the revision. Patients typically wear a sling for several weeks and begin supervised physical therapy early in the healing process. Pain relief often improves gradually, and regaining strength and motion may take several months. Close follow-up with the orthopaedic team is essential to monitor healing and long-term function.
Quick Links
- Shoulder Anatomy
- Arthritis of the Shoulder
- Rotator Cuff Tear
- Shoulder Dislocation
- Frozen Shoulder
- Shoulder Instability
- Shoulder Fracture
- Biceps Tendon Rupture
- Shoulder Arthroscopy
- Total Shoulder Replacement
- Reverse Shoulder Replacement
- Shoulder Hemiarthroplasty
- Rotator Cuff Repair
- Shoulder Stabilization





