Total Shoulders with Inlay Glenoids
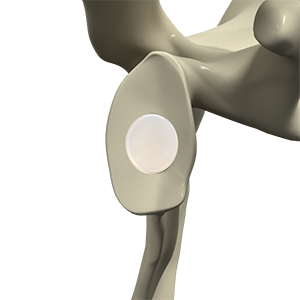
Total shoulders with inlay glenoid implant represent an advanced approach to total shoulder arthroplasty designed to ideally improve implant durability and reduce complications related to glenoid implant wear. In this technique, the glenoid (socket) component is placed flush within the bone rather than sitting on top of it. This design may help decrease edge loading, reduce loosening risk and better preserve bone stock, particularly in active patients.
What Is a Total Shoulder with an Inlay Glenoid?
A total shoulder with an inlay glenoid is a form of anatomic total shoulder replacement in which the humeral head (ball) is replaced with a metal implant and the glenoid component is recessed into the socket bone. Unlike traditional onlay glenoid implants that sit on the surface of the bone, inlay designs are countersunk within the glenoid. This positioning aims to reduce stress at the implant-bone interface and improve long-term stability.
Anatomy
The shoulder is a ball-and-socket joint composed of:
- The humeral head (ball)
- The glenoid (socket) of the shoulder blade
- Articular cartilage that cushions movement
- The rotator cuff muscles and tendons
- The joint capsule and surrounding ligaments
In a healthy shoulder, the rotator cuff centers the humeral head within the glenoid during motion. Proper implant positioning is essential to restore normal joint mechanics and maintain stability.
Pathology
Total shoulder replacement with an inlay glenoid is typically performed for advanced glenohumeral arthritis. Over time, cartilage loss leads to bone-on-bone contact, causing pain, stiffness, grinding and limited range of motion. Some patients also develop glenoid bone wear or deformity. The inlay design may help address certain wear patterns while preserving more native bone compared to traditional techniques.
When Is a Total Shoulder with an Inlay Glenoid Recommended?
This procedure may be recommended when non-surgical treatments fail and the patient has:
- Advanced primary osteoarthritis of the shoulder
- Intact and functional rotator cuff tendons
- Glenoid wear that may benefit from bone-preserving techniques
- Persistent pain affecting daily activities and sleep
- Adequate bone quality to support an inlay implant
A detailed clinical exam and imaging studies help determine if this approach is appropriate.
What Does Preparation for a Total Shoulder with an Inlay Glenoid Involve?
Preparation includes a comprehensive orthopaedic evaluation and imaging, often including CT scans to assess glenoid bone shape and version. Risk stratification may be required. Patients receive education about the surgical plan, postoperative sling use, and rehabilitation expectations. Planning for temporary assistance at home is advised.
How Is a Total Shoulder with an Inlay Glenoid Performed?
The procedure is performed under anesthesia through an incision at the front of the shoulder. The damaged humeral head is replaced with a metal component. The glenoid is carefully prepared, and the inlay implant is recessed flush within the bone. Precise alignment is critical to restore smooth motion and joint balance. The incision is then closed, and the arm is placed in a sling.
What to Expect During Recovery After a Total Shoulder with an Inlay Glenoid?
Recovery follows a structured rehabilitation plan. A sling is worn for several weeks, with early passive motion exercises guided by a physical therapist. Gradual strengthening begins as healing progresses. Most patients experience significant pain relief and improved range of motion over four to six months, with continued functional gains thereafter.
Quick Links
- Shoulder Anatomy
- Arthritis of the Shoulder
- Rotator Cuff Tear
- Shoulder Dislocation
- Frozen Shoulder
- Shoulder Instability
- Shoulder Fracture
- Biceps Tendon Rupture
- Shoulder Arthroscopy
- Total Shoulder Replacement
- Reverse Shoulder Replacement
- Shoulder Hemiarthroplasty
- Rotator Cuff Repair
- Shoulder Stabilization





